

At Haven, he wasn't just another patient; he was a partner in his care. This means you can access your specialist from anywhere, reducing the need for stressful commutes that can trigger migraines. Haven's platform is designed with your convenience in mind, allowing you to book appointments directly from your home. Learn more about Haven Headache & Migraine Center here. Moreover, we're exploring innovative technologies and methodologies that promise more personalized migraine management strategies. Learn more about California Migraine Expert Board-Certified here We're committed to translating our research findings into practical, accessible treatments that offer real relief.
They listen to your story, taking into account every detail that could influence your treatment plan. You're now able to receive specialized care from the comfort of your home, eliminating the need for stressful commutes and long waits in clinical settings. In essence, telehealth services not only make your life easier but can also enhance the quality of your migraine and headache care. From the bustling streets of Los Angeles to the serene landscapes of the Napa Valley, we're on a mission to ensure that anyone suffering from migraines can access compassionate, effective care.
We know that living with migraines can feel isolating, but you're not alone. Headache Disorder Treatment One patient, Sarah, had suffered debilitating migraines for years, finding little relief from traditional in-person visits. Navigating the path to migraine relief doesn't end with lifestyle changes; ongoing support plays a pivotal role in managing this condition effectively. That's why they've strategically placed their centers across California Migraine Expert Board-Certified, ensuring that you're never too far from expert care.
How does Haven Headache & Migraine Center ensure that living far from their California Migraine Expert Board-Certified location isn't a barrier to accessing their specialized care? They offer flexible appointment times, including early mornings, late evenings, and weekends, accommodating your unique needs and lifestyle. They'll also factor in any underlying conditions that could be impacting your migraines. You'll have access to devices that can adjust your environment to reduce triggers, such as lighting and temperature, creating a personal safe haven wherever you go.
Whether you're juggling a busy schedule, living in a remote area, or facing mobility issues, telehealth bridges the gap, ensuring you get the support you need when you need it. Your journey doesn't end with the creation of your treatment plan. It's a dynamic, responsive system that puts your needs at the forefront, making your telehealth experience as effective and personalized as possible. After scheduling your appointment online, you'll receive a comprehensive evaluation, where specialists delve into your medical history, symptom patterns, and lifestyle factors. First off, let's talk about your diet.
This convenience means you can have your consultation wherever you're most comfortable, without the stress of traveling. With the integration of artificial intelligence and machine learning, doctors will have tools at their disposal to predict potential triggers and prevent attacks before they start. Neurologists Near Me Haven's telehealth services offer a convenient, cutting-edge approach to accessing specialized headache care, without the need to leave your home. Sharing stories and solutions can inspire and empower you to take control of your migraines in ways you mightn't have considered before.
It's easier than you might think. Building on the foundation of an expert team, Haven Headache & Migraine Center offers you access to the latest in migraine treatment advancements. It's a comprehensive evaluation aimed at understanding the full scope of your condition. Join us, and let's tackle migraines together. Read more about California Migraine Expert Board-Certified here
These might encompass biofeedback, where you learn to control certain body functions to reduce headache frequency, or acupuncture, which has been shown to relieve some types of pain and stress. It's also helpful to list your current medications and any questions or concerns you have. At Haven Headache & Migraine Center, we understand how vital it's for you to receive the care you need without unnecessary stress. Write down a description of your symptoms, including when they started, their frequency, and what, if anything, seems to trigger them.
The Greater Los Angeles and San Francisco Bay areas are the nation's second- and fifth-most populous urban regions, with 19 million and 10 million residents respectively. Los Angeles is the state's most populous city and the nation's second-most. California's capital is Sacramento. Part of the Californias region of North America, the state's diverse geography ranges from the Pacific Coast and metropolitan areas in the west to the Sierra Nevada mountains in the east, and from the redwood and Douglas fir forests in the northwest to the Mojave Desert in the southeast. Two-thirds of the nation's earthquake risk lies in California. The Central Valley, a fertile agricultural area, dominates the state's center. The large size of the state results in climates that vary from moist temperate rainforest in the north to arid desert in the interior, as well as snowy alpine in the mountains. Droughts and wildfires are an ongoing issue,[13] while simultaneously, atmospheric rivers are turning increasingly prevalent and leading to intense flooding events—especially in the winter.
Dive into our resources today and take a significant step towards taking control of your migraines. You're no longer caught in traffic, worried about being late for an appointment, or standing in long lines.


Understanding your migraines is the first step towards managing them. So, you're not just getting standard care; you're benefiting from the latest in migraine management, all from the comfort of your home.
First, you'll receive a confirmation email with all the necessary details, including a link to your virtual consultation. Imagine wearable devices that not only track your daily activities but also predict migraines before they start, allowing for preemptive treatment. You're not left to navigate the plan alone; regular virtual check-ins allow for adjustments based on how you're responding to the treatment. They aim to make their services accessible, ensuring cost doesn't prevent anyone from getting the help they need. You're now at the forefront of a revolution in migraine management, where innovation meets individual care.

First, we'll help you understand your insurance policy's specifics. Pain Relief Specialists This approach not only overcomes traditional barriers but also empowers you to take control of your health journey. It's designed to be intuitive, so you're not left feeling frustrated or confused. Migraine Diagnosis You'll have the opportunity to track your migraine patterns and symptoms, sharing them with your provider in real-time, which is vital for adjusting treatment plans to best suit your needs. Take Sarah's journey, for instance.
You no longer need to endure long commutes or wait in crowded lobbies. Stick around, and you'll discover the remarkable ways in which Haven Headache & Migraine Center is revolutionizing migraine care statewide.
These stories highlight just how life-changing telemedicine can be for those battling chronic headaches and migraines. Initiating your journey with Haven Headache & Migraine Center is a straightforward process designed to swiftly address your unique needs. AI will analyze your health data to predict patterns and recommend adjustments to your treatment plan, ensuring it remains as effective as possible over time. Instead, you can access top-notch headache and migraine care right from your home. Imagine being plagued by migraines so severe you can't leave your bed, let alone drive to a doctor's appointment.
They can offer guidance, adjust your treatment plan as needed, and introduce you to new management strategies as they become available. By staying informed, you can make empowered decisions about your health and wellness. These signs can vary but often include yawning, irritability, and a stiff neck. Beyond securing your data, Haven Headache & Migraine Center leverages advanced technology to enhance your telehealth experience.
You're not alone. If you're caught in the grips of migraines, let these stories remind you: relief isn't just possible; it's within reach at Haven Headache & Migraine Center. It's a condition that demands attention and understanding because what triggers a migraine in you could be completely different from what triggers it in someone else. Haven's approach combines the rise of telehealth with personalized care plans, promising an intriguing blend of convenience, customization, and ongoing support.
Building on the foundation laid by our expert team, let's explore how real patients have achieved remarkable relief from their migraines at Haven Headache & Migraine Center. Our approach combines the latest in medical advancements with holistic methods to address your migraines from every angle. This method isn't just about treating symptoms; it's about understanding the root cause of your pain and crafting a tailored plan that addresses your specific needs. This personalized approach ensures that your care plan is as unique as your migraine patterns.
| Migraine | |
|---|---|
 |
|
| Woman during a migraine attack | |
| Specialty | Neurology |
| Symptoms | Headaches coupled with sensory disturbances such as nausea, sensitivity to light, sound, and smell |
| Usual onset | Around puberty |
| Duration | Recurrent, long term |
| Causes | Environmental and genetic |
| Risk factors | Family history, female sex |
| Differential diagnosis | Subarachnoid hemorrhage, venous thrombosis, idiopathic intracranial hypertension, brain tumor, tension headache, sinusitis, cluster headache |
| Prevention | Propranolol, amitriptyline, topiramate, calcitonin gene-related peptide receptor antagonists (CGRPs) |
| Medication | Ibuprofen, paracetamol (acetaminophen), triptans, ergotamines |
| Prevalence | ~15% |
Migraine ( UK: /ˈmiËÂÂÉ¡reɪn/,
US: /ˈmaɪ-/)[1][2] is a complex neurological disorder characterized by episodes of moderate-to-severe headache, most often unilateral and generally associated with nausea, and light and sound sensitivity.[3][4] Other characterizing symptoms may include vomiting, cognitive dysfunction, allodynia, and dizziness.[3] Exacerbation or worsening of headache symptoms during physical activity is another distinguishing feature.[5]
Up to one-third of people with migraine experience aura, a premonitory period of sensory disturbance widely accepted to be caused by cortical spreading depression at the onset of a migraine attack.[4] Although primarily considered to be a headache disorder, migraine is highly heterogenous in its clinical presentation and is better thought of as a spectrum disease rather than a distinct clinical entity.[6] Disease burden can range from episodic discrete attacks to chronic disease.[6][7]
Migraine is believed to be caused by a mixture of environmental and genetic factors that influence the excitation and inhibition of nerve cells in the brain.[8] The accepted hypothesis suggests that multiple primary neuronal impairments lead to a series of intracranial and extracranial changes, triggering a physiological cascade that leads to migraine symptomatology.[9]
Initial recommended treatment for acute attacks is with over-the-counter analgesics (pain medication) such as ibuprofen and paracetamol (acetaminophen) for headache, antiemetics (anti-nausea medication) for nausea, and the avoidance of migraine triggers.[10] Specific medications such as triptans, ergotamines, or calcitonin gene-related peptide receptor antagonist (CGRP) inhibitors may be used in those experiencing headaches that do not respond to the over-the-counter pain medications.[11] For people who experience four or more attacks per month, or could otherwise benefit from prevention, prophylactic medication is recommended.[12] Commonly prescribed prophylactic medications include beta blockers like propranolol, anticonvulsants like sodium valproate, antidepressants like amitriptyline, and other off-label classes of medications.[13] Preventive medications inhibit migraine pathophysiology through various mechanisms, such as blocking calcium and sodium channels, blocking gap junctions, and inhibiting matrix metalloproteinases, among other mechanisms.[14][15] Non-pharmacological preventive therapies include nutritional supplementation, dietary interventions, sleep improvement, and aerobic exercise.[16] In 2018, the first medication (Erenumab) of a new class of drugs specifically designed for migraine prevention called calcitonin gene-related peptide receptor antagonists (CGRPs) was approved by the FDA.[17] As of July 2023, the FDA has approved eight drugs that act on the CGRP system for use in the treatment of migraine.[18]
Globally, approximately 15% of people are affected by migraine.[19] In the Global Burden of Disease Study, conducted in 2010, migraine ranked as the third-most prevalent disorder in the world.[20] It most often starts at puberty and is worst during middle age.[21] As of 2016[update], it is one of the most common causes of disability.[22]
Migraine typically presents with self-limited, recurrent severe headaches associated with autonomic symptoms.[23][24] About 15–30% of people living with migraine experience episodes with aura,[10][25] and they also frequently experience episodes without aura.[26] The severity of the pain, duration of the headache, and frequency of attacks are variable.[23] A migraine attack lasting longer than 72 hours is termed status migrainosus.[27] There are four possible phases to a migraine attack, although not all the phases are necessarily experienced:[28]
Migraine is associated with major depression, bipolar disorder, anxiety disorders, and obsessive–compulsive disorder. These psychiatric disorders are approximately 2–5 times more common in people without aura, and 3–10 times more common in people with aura.[29]
Prodromal or premonitory symptoms occur in about 60% of those with migraine,[30][31] with an onset that can range from two hours to two days before the start of pain or the aura.[32] These symptoms may include a wide variety of phenomena,[33] including altered mood, irritability, depression or euphoria, fatigue, craving for certain food(s), stiff muscles (especially in the neck), constipation or diarrhea, and sensitivity to smells or noise.[31] This may occur in those with either migraine with aura or migraine without aura.[34] Neuroimaging indicates the limbic system and hypothalamus as the origin of prodromal symptoms in migraine.[35]
 |
 |
 |
 |
Aura is a transient focal neurological phenomenon that occurs before or during the headache.[30] Aura appears gradually over a number of minutes (usually occurring over 5–60 minutes) and generally lasts less than 60 minutes.[36][37] Symptoms can be visual, sensory or motoric in nature, and many people experience more than one.[38] Visual effects occur most frequently: they occur in up to 99% of cases, and in more than 50% of cases are not accompanied by sensory or motor effects.[38] If any symptom remains after 60 minutes, the state is known as persistent aura.[39]
Visual disturbances often consist of a scintillating scotoma (an area of partial alteration in the field of vision which flickers and may interfere with a person's ability to read or drive).[30] These typically start near the center of vision and then spread out to the sides with zigzagging lines, which have been described as looking like fortifications or walls of a castle.[38] Usually, the lines are in black and white, but some people also see colored lines.[38] Some people lose part of their field of vision known as hemianopsia while others experience blurring.[38]
Sensory auras are the second most common type; they occur in 30–40% of people with auras.[38] Often, a feeling of pins-and-needles begins on one side in the hand and arm and spreads to the nose–mouth area on the same side.[38] Numbness usually occurs after the tingling has passed with a loss of position sense.[38] Other symptoms of the aura phase can include speech or language disturbances, world spinning, and, less commonly, motor problems.[38] Motor symptoms indicate that this is a hemiplegic migraine, and weakness often lasts longer than one hour unlike other auras.[38] Auditory hallucinations or delusions have also been described.[40]
Classically the headache is unilateral, throbbing, and moderate to severe in intensity.[36] It usually comes on gradually[36] and is aggravated by physical activity during a migraine attack.[28] However, the effects of physical activity on migraine are complex, and some researchers have concluded that, while exercise can trigger migraine attacks, regular exercise may have a prophylactic effect and decrease frequency of attacks.[41] The feeling of pulsating pain is not in phase with the pulse.[42] In more than 40% of cases, however, the pain may be bilateral (both sides of the head), and neck pain is commonly associated with it.[43] Bilateral pain is particularly common in those who have migraine without aura.[30] Less commonly pain may occur primarily in the back or top of the head.[30] The pain usually lasts 4 to 72 hours in adults;[36] however, in young children frequently lasts less than 1 hour.[44] The frequency of attacks is variable, from a few in a lifetime to several a week, with the average being about one a month.[45][46]
The pain is frequently accompanied by nausea, vomiting, sensitivity to light, sensitivity to sound, sensitivity to smells, fatigue, and irritability.[30] Many thus seek a dark and quiet room.[47] In a basilar migraine, a migraine with neurological symptoms related to the brain stem or with neurological symptoms on both sides of the body,[48] common effects include a sense of the world spinning, light-headedness, and confusion.[30] Nausea occurs in almost 90% of people, and vomiting occurs in about one-third.[47] Other symptoms may include blurred vision, nasal stuffiness, diarrhea, frequent urination, pallor, or sweating.[49] Swelling or tenderness of the scalp may occur as can neck stiffness.[49] Associated symptoms are less common in the elderly.[50]
Sometimes, aura occurs without a subsequent headache.[38] This is known in modern classification as a typical aura without headache, or acephalgic migraine in previous classification, or commonly as a silent migraine.[51][52] However, silent migraine can still produce debilitating symptoms, with visual disturbance, vision loss in half of both eyes, alterations in color perception, and other sensory problems, like sensitivity to light, sound, and odors.[53] It can last from 15 to 30 minutes, usually no longer than 60 minutes, and it can recur or appear as an isolated event.[54] Many report a sore feeling in the area where the migraine was, and some report impaired thinking for a few days after the headache has passed. The person may feel tired or "hung over" and have head pain, cognitive difficulties, gastrointestinal symptoms, mood changes, and weakness.[55] According to one summary, "Some people feel unusually refreshed or euphoric after an attack, whereas others note depression and malaise."[56][unreliable medical source?]
The underlying cause of migraine is unknown.[57] However, it is believed to be related to a mix of environmental and genetic factors.[8] Migraine runs in families in about two-thirds of cases[23] and rarely occur due to a single gene defect.[58] While migraine attacks were once believed to be more common in those of high intelligence, this does not appear to be true.[45] A number of psychological conditions are associated, including depression, anxiety, and bipolar disorder.[59]

Success of the surgical migraine treatment by decompression of extracranial sensory nerves adjacent to vessels[60] suggests that people with migraine may have anatomical predisposition for neurovascular compression[61] that may be caused by both intracranial and extracranial vasodilation due to migraine triggers.[62] This, along with the existence of numerous cranial neural interconnections,[63] may explain the multiple cranial nerve involvement and consequent diversity of migraine symptoms.[64]
Studies of twins indicate a 34–51% genetic influence on the likelihood of developing migraine.[8] This genetic relationship is stronger for migraine with aura than for migraine without aura.[26] It is clear from family and populations studies that migraine is a complex disorder, where numerous genetic risk variants exist, and where each variant increases the risk of migraine marginally.[65][66] It is also known that having several of these risk variants increases the risk by a small to moderate amount.[58]
Single gene disorders that result in migraine are rare.[58] One of these is known as familial hemiplegic migraine, a type of migraine with aura, which is inherited in an autosomal dominant fashion.[67][68] Four genes have been shown to be involved in familial hemiplegic migraine.[69] Three of these genes are involved in ion transport.[69] The fourth is the axonal protein PRRT2, associated with the exocytosis complex.[69] Another genetic disorder associated with migraine is CADASIL syndrome or cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy.[30] One meta-analysis found a protective effect from angiotensin converting enzyme polymorphisms on migraine.[70] The TRPM8 gene, which codes for a cation channel, has been linked to migraine.[71]
The common forms of migraine are polygenetic, where common variants of numerous genes contribute to the predisposition for migraine. These genes can be placed in three categories, increasing the risk of migraine in general, specifically migraine with aura, or migraine without aura.[72][73] Three of these genes, CALCA, CALCB, and HTR1F are already target for migraine specific treatments. Five genes are specific risk to migraine with aura, PALMD, ABO, LRRK2, CACNA1A and PRRT2, and 13 genes are specific to migraine without aura. Using the accumulated genetic risk of the common variations, into a so-called polygenetic risk, it is possible to assess e.g. the treatment response to triptans.[74][75]
Migraine may be induced by triggers, with some reporting it as an influence in a minority of cases[23] and others, the majority.[76] Many things, such as fatigue, certain foods, alcohol, and weather, have been labeled as triggers; however, the strength and significance of these relationships are uncertain.[76][77] Most people with migraine report experiencing triggers.[78] Symptoms may start up to 24 hours after a trigger.[23]
Also, evidence shows a strong association between migraine and the quality of sleep, particularly poor subjective quality of sleep. The relationship seems to be bidirectional, as migraine frequency increases with low quality of sleep, yet the underlying mechanism of this correlation remains poorly understood.[79]
Common triggers quoted are stress, hunger, and fatigue (these equally contribute to tension headaches).[76] Psychological stress has been reported as a factor by 50–80% of people.[80] Migraine has also been associated with post-traumatic stress disorder and abuse.[81] Migraine episodes are more likely to occur around menstruation.[80] Other hormonal influences, such as menarche, oral contraceptive use, pregnancy, perimenopause, and menopause, also play a role.[82] These hormonal influences seem to play a greater role in migraine without aura.[45] Migraine episodes typically do not occur during the second and third trimesters of pregnancy, or following menopause.[30]
Between 12% and 60% of people report foods as triggers.[83][84]
There are many reports[85][86][87][88][89] that tyramine – which is naturally present in chocolate, alcoholic beverages, most cheeses, processed meats, and other foods – can trigger migraine symptoms in some individuals. Monosodium glutamate (MSG) has been reported as a trigger for migraine,[90] but a systematic review concluded that "a causal relationship between MSG and headache has not been proven... It would seem premature to conclude that the MSG present in food causes headache".[91]
Migraines may be triggered by weather changes, including changes in temperature and barometric pressure.[92][93]
A 2009 review on potential triggers in the indoor and outdoor environment previously concluded that while there were insufficient studies to confirm environmental factors as causing migraine, "migraineurs worldwide consistently report similar environmental triggers ... such as barometric pressure change, bright sunlight, flickering lights, air quality and odors".[94]
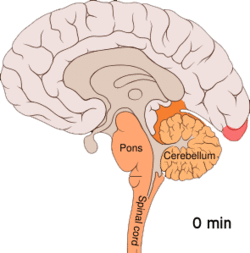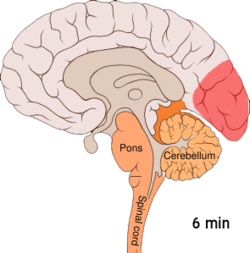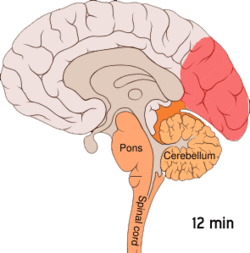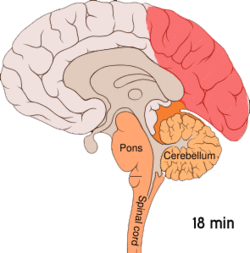
Migraine is believed to be primarily a neurological disorder,[95][96] while others believe it to be a neurovascular disorder with blood vessels playing the key role, although evidence does not support this completely.[97][98][99][100] Others believe both are likely important.[101][102][103][104] One theory is related to increased excitability of the cerebral cortex and abnormal control of pain neurons in the trigeminal nucleus of the brainstem.[105]
Sensitization of trigeminal pathways is a key pathophysiological phenomenon in migraine. It is debatable whether sensitization starts in the periphery or in the brain.[106][107]
Cortical spreading depression, or spreading depression according to Leão, is a burst of neuronal activity followed by a period of inactivity, which is seen in those with migraine with aura.[108] There are several explanations for its occurrence, including activation of NMDA receptors leading to calcium entering the cell.[108] After the burst of activity, the blood flow to the cerebral cortex in the affected area is decreased for two to six hours.[108] It is believed that when depolarization travels down the underside of the brain, nerves that sense pain in the head and neck are triggered.[108]
The exact mechanism of the head pain which occurs during a migraine episode is unknown.[109] Some evidence supports a primary role for central nervous system structures (such as the brainstem and diencephalon),[110] while other data support the role of peripheral activation (such as via the sensory nerves that surround blood vessels of the head and neck).[109] The potential candidate vessels include dural arteries, pial arteries and extracranial arteries such as those of the scalp.[109] The role of vasodilatation of the extracranial arteries, in particular, is believed to be significant.[111]
Adenosine, a neuromodulator, may be involved.[112] Released after the progressive cleavage of adenosine triphosphate (ATP), adenosine acts on adenosine receptors to put the body and brain in a low activity state by dilating blood vessels and slowing the heart rate, such as before and during the early stages of sleep. Adenosine levels are high during migraine attacks.[112][113] Caffeine's role as an inhibitor of adenosine may explain its effect in reducing migraine.[114] Low levels of the neurotransmitter serotonin, also known as 5-hydroxytryptamine (5-HT), are also believed to be involved.[115]
Calcitonin gene-related peptides (CGRPs) have been found to play a role in the pathogenesis of the pain associated with migraine, as levels of it become elevated during an attack.[10][42]
The diagnosis of a migraine is based on signs and symptoms.[23] Neuroimaging tests are not necessary to diagnose migraine, but may be used to find other causes of headaches in those whose examination and history do not confirm a migraine diagnosis.[116] It is believed that a substantial number of people with the condition remain undiagnosed.[23]
The diagnosis of migraine without aura, according to the International Headache Society, can be made according to the "5, 4, 3, 2, 1 criteria", which is as follows:[28]
If someone experiences two of the following: photophobia, nausea, or inability to work or study for a day, the diagnosis is more likely.[117] In those with four out of five of the following: pulsating headache, duration of 4–72 hours, pain on one side of the head, nausea, or symptoms that interfere with the person's life, the probability that this is a migraine attack is 92%.[10] In those with fewer than three of these symptoms, the probability is 17%.[10]
Migraine was first comprehensively classified in 1988.[26]
The International Headache Society updated their classification of headaches in 2004.[28] A third version was published in 2018.[118] According to this classification, migraine is a primary headache disorder along with tension-type headaches and cluster headaches, among others.[119]
Migraine is divided into six subclasses (some of which include further subdivisions):[120]
The diagnosis of abdominal migraine is controversial.[122] Some evidence indicates that recurrent episodes of abdominal pain in the absence of a headache may be a type of migraine[122][123] or are at least a precursor to migraine attacks.[26] These episodes of pain may or may not follow a migraine-like prodrome and typically last minutes to hours.[122] They often occur in those with either a personal or family history of typical migraine.[122] Other syndromes that are believed to be precursors include cyclical vomiting syndrome and benign paroxysmal vertigo of childhood.[26]
Other conditions that can cause similar symptoms to a migraine headache include temporal arteritis, cluster headaches, acute glaucoma, meningitis and subarachnoid hemorrhage.[10] Temporal arteritis typically occurs in people over 50 years old and presents with tenderness over the temple, cluster headache presents with one-sided nose stuffiness, tears and severe pain around the orbits, acute glaucoma is associated with vision problems, meningitis with fevers, and subarachnoid hemorrhage with a very fast onset.[10] Tension headaches typically occur on both sides, are not pounding, and are less disabling.[10]
Those with stable headaches that meet criteria for migraine should not receive neuroimaging to look for other intracranial disease.[124][125][126] This requires that other concerning findings such as papilledema (swelling of the optic disc) are not present. People with migraine are not at an increased risk of having another cause for severe headaches.[citation needed]
Management of migraine includes prevention of migraine attacks and rescue treatment. There are three main aspects of treatment: trigger avoidance, acute (abortive), and preventive (prophylactic) control.[127]
Modern approaches to migraine management emphasize personalized care that considers individual patient needs. Lifestyle modifications, such as managing triggers and addressing comorbidities, form the foundation of treatment. Behavioral techniques and supplements like magnesium and riboflavin can serve as supportive options for some individuals.[128] Behavioral techniques that have been utilized in the treatment of migraines include Cognitive Behavioral Therapy (CBT), relaxation training, biofeedback, Acceptance and Commitment Therapy (ACT), as well as mindfulness-based therapies.[129] A 2024 systematic literature review and meta analysis found evidence that treatments such as CBT, relaxation training, ACT, and mindfulness-based therapies can reduce migraine frequency both on their own and in combination with other treatment options.[129] In addition, it was found that relaxation therapy aided in the lessening of migraine frequency when compared to education by itself.[129] Similarly, for children and adolescents, CBT and biofeedback strategies are effective in decreasing of frequency and intensity of migraines. These techniques often include relaxation methods and promotion of long-term management without medication side effects, which is emphasized for younger individuals.[129] Acute treatments, including NSAIDs and triptans, are most effective when administered early in an attack, while preventive medications are recommended for those experiencing frequent or severe migraines. Proven preventive options include beta blockers, topiramate, and CGRP inhibitors like erenumab and galcanezumab, which have demonstrated significant efficacy in clinical studies.[130] The European Consensus Statement provides a framework for diagnosis and management, emphasizing the importance of accurate assessment, patient education, and consistent adherence to prescribed treatments. Innovative therapies of oral medications used to treat migraine symptoms, such as gepants and ditans, are emerging as alternatives for patients who cannot use traditional options.[131]
A 2024 systematic review and network meta analysis compared the effectiveness of medications for acute migraine attacks in adults. It found that triptans were the most effective class of drugs, followed by non-steroidal anti-inflammatories. Gepants were less effective than non-steroidal anti-inflammatory drugs.[132][133]
Calcitonin gene-related peptide (CGRP) is a neuropeptide implicated in the pathophysiology of migraines. It is predominantly found in the trigeminal ganglion and central nervous system pathways associated with migraine mechanisms.[134] During migraine attacks, elevated levels of CGRP are detected, leading to vasodilation of cerebral and dural blood vessels and the release of inflammatory mediators from mast cells. These actions contribute to the transmission of nociceptive signals, culminating in migraine pain. Targeting CGRP has emerged as a promising therapeutic strategy for migraine management.[medical citation needed]
"Migraine exists on a continuum of different attack frequencies and associated levels of disability."[135] For those with occasional, episodic migraine, a "proper combination of drugs for prevention and treatment of migraine attacks" can limit the disease's impact on patients' personal and professional lives.[136] But fewer than half of people with migraine seek medical care and more than half go undiagnosed and undertreated.[137] "Responsive prevention and treatment of migraine is incredibly important" because evidence shows "an increased sensitivity after each successive attack, eventually leading to chronic daily migraine in some individuals."[136] Repeated migraine results in "reorganization of brain circuitry", causing "profound functional as well as structural changes in the brain."[138] "One of the most important problems in clinical migraine is the progression from an intermittent, self-limited inconvenience to a life-changing disorder of chronic pain, sensory amplification, and autonomic and affective disruption. This progression, sometimes termed chronification in the migraine literature, is common, affecting 3% of migraineurs in a given year, such that 8% of migraineurs have chronic migraine in any given year." Brain imagery reveals that the electrophysiological changes seen during an attack become permanent in people with chronic migraine; "thus, from an electrophysiological point of view, chronic migraine indeed resembles a never-ending migraine attack."[138] Severe migraine ranks in the highest category of disability, according to the World Health Organization, which uses objective metrics to determine disability burden for the authoritative annual Global Burden of Disease report. The report classifies severe migraine alongside severe depression, active psychosis, quadriplegia, and terminal-stage cancer.[139]
Migraine with aura appears to be a risk factor for ischemic stroke[140] doubling the risk.[141] Being a young adult, being female, using hormonal birth control, and smoking further increases this risk.[140] There also appears to be an association with cervical artery dissection.[142] Migraine without aura does not appear to be a factor.[143] The relationship with heart problems is inconclusive with a single study supporting an association.[140] Migraine does not appear to increase the risk of death from stroke or heart disease.[144] Preventative therapy of migraine in those with migraine with aura may prevent associated strokes.[145] People with migraine, particularly women, may develop higher than average numbers of white matter brain lesions of unclear significance.[146]

Migraine is common, with around 33% of women and 18% of men affected at some point in their lifetime.[147] Onset can be at any age, but prevalence rises sharply around puberty, and remains high until declining after age 50.[147] Before puberty, boys and girls are equally impacted, with around 5% of children experiencing migraine attacks. From puberty onwards, women experience migraine attacks at greater rates than men. From age 30 to 50, up to 4 times as many women experience migraine attacks as men;[147] this is most pronounced in migraine without aura.[148]
Worldwide, migraine affects nearly 15% or approximately one billion people.[19] In the United States, about 6% of men and 18% of women experience a migraine attack in a given year, with a lifetime risk of about 18% and 43%, respectively.[23] In Europe, migraine affects 12–28% of people at some point in their lives, with about 6–15% of adult men and 14–35% of adult women getting at least one attack yearly.[149] Rates of migraine are slightly lower in Asia and Africa than in Western countries.[45][150] Chronic migraine occurs in approximately 1.4–2.2% of the population.[151]
During perimenopause symptoms often get worse before decreasing in severity.[152] While symptoms resolve in about two-thirds of the elderly, in 3–10% they persist.[50]

An early description consistent with migraine is contained in the Ebers Papyrus, written around 1500 BCE in ancient Egypt.[153]
The word migraine is from the Greek ἡμικρá¾±νίᾱ (hÄ“mikrÄÂÂníÄÂÂ), 'pain in half of the head',[154] from ἡμι- (hÄ“mi-), 'half' and κρá¾±νίον (krÄÂÂníon), 'skull'.[155]
In 200 BCE, writings from the Hippocratic school of medicine described the visual aura that can precede the headache and a partial relief occurring through vomiting.[156]
A second-century description by Aretaeus of Cappadocia divided headaches into three types: cephalalgia, cephalea, and heterocrania.[157] Galen of Pergamon used the term hemicrania (half-head), from which the word migraine was eventually derived.[157] Galen also proposed that the pain arose from the meninges and blood vessels of the head.[156] Migraine was first divided into the two now used types – migraine with aura (migraine ophthalmique) and migraine without aura (migraine vulgaire) in 1887 by Louis Hyacinthe Thomas, a French librarian.[156] The mystical visions of Hildegard von Bingen, which she described as "reflections of the living light", are consistent with the visual aura experienced during migraine attacks.[158]

Trepanation, the deliberate drilling of holes into a skull, was practiced as early as 7,000 BCE.[153] While sometimes people survived, many would have died from the procedure due to infection.[159] It was believed to work via "letting evil spirits escape".[160] William Harvey recommended trepanation as a treatment for migraine in the 17th century.[161] The association between trepanation and headaches in ancient history may simply be a myth or unfounded speculation that originated several centuries later. In 1913, the world-famous American physician William Osler misinterpreted the French anthropologist and physician Paul Broca's words about a set of children's skulls from the Neolithic age that he found during the 1870s. These skulls presented no evident signs of fractures that could justify this complex surgery for mere medical reasons. Trepanation was probably born of superstitions, to remove "confined demons" inside the head, or to create healing or fortune talismans with the bone fragments removed from the skulls of the patients. However, Osler wanted to make Broca's theory more palatable to his modern audiences, and explained that trepanation procedures were used for mild conditions such as "infantile convulsions headache and various cerebral diseases believed to be caused by confined demons."[162]
While many treatments for migraine have been attempted, it was not until 1868 that use of a substance which eventually turned out to be effective began.[156] This substance was the fungus ergot from which ergotamine was isolated in 1918[163] and first used to treat migraine in 1925.[164] Methysergide was developed in 1959 and the first triptan, sumatriptan, was developed in 1988.[163] During the 20th century, with better study design, effective preventive measures were found and confirmed.[156]
Migraine is a significant source of both medical costs and lost productivity. It has been estimated that migraine is the most costly neurological disorder in the European Community, costing more than €27 billion per year.[165] In the United States, direct costs have been estimated at $17 billion, while indirect costs – such as missed or decreased ability to work – is estimated at $15 billion.[166] Nearly a tenth of the direct cost is due to the cost of triptans.[166] In those who do attend work during a migraine attack, effectiveness is decreased by around a third.[165] Negative impacts also frequently occur for a person's family.[165]
Transcranial magnetic stimulation shows promise,[10][167] as does transcutaneous supraorbital nerve stimulation.[168] There is preliminary evidence that a ketogenic diet may help prevent episodic and long-term migraine.[169][170]
Statistical data indicates that women may be more prone to having migraine, showing migraine incidence three times higher among women than men.[171][172] The Society for Women's Health Research has also mentioned hormonal influences, mainly estrogen, as having a considerable role in provoking migraine pain. Studies and research related to the sex dependencies of migraine are ongoing, and conclusions have yet to be achieved.[173]
Disability classes for the Global Burden of Disease study (table 8)
| External audio | |
|---|---|
| Migraine | |
|---|---|
 |
|
| Woman during a migraine attack | |
| Specialty | Neurology |
| Symptoms | Headaches coupled with sensory disturbances such as nausea, sensitivity to light, sound, and smell |
| Usual onset | Around puberty |
| Duration | Recurrent, long term |
| Causes | Environmental and genetic |
| Risk factors | Family history, female sex |
| Differential diagnosis | Subarachnoid hemorrhage, venous thrombosis, idiopathic intracranial hypertension, brain tumor, tension headache, sinusitis, cluster headache |
| Prevention | Propranolol, amitriptyline, topiramate, calcitonin gene-related peptide receptor antagonists (CGRPs) |
| Medication | Ibuprofen, paracetamol (acetaminophen), triptans, ergotamines |
| Prevalence | ~15% |
Migraine ( UK: /ˈmiËÂÂÉ¡reɪn/,
US: /ˈmaɪ-/)[1][2] is a complex neurological disorder characterized by episodes of moderate-to-severe headache, most often unilateral and generally associated with nausea, and light and sound sensitivity.[3][4] Other characterizing symptoms may include vomiting, cognitive dysfunction, allodynia, and dizziness.[3] Exacerbation or worsening of headache symptoms during physical activity is another distinguishing feature.[5]
Up to one-third of people with migraine experience aura, a premonitory period of sensory disturbance widely accepted to be caused by cortical spreading depression at the onset of a migraine attack.[4] Although primarily considered to be a headache disorder, migraine is highly heterogenous in its clinical presentation and is better thought of as a spectrum disease rather than a distinct clinical entity.[6] Disease burden can range from episodic discrete attacks to chronic disease.[6][7]
Migraine is believed to be caused by a mixture of environmental and genetic factors that influence the excitation and inhibition of nerve cells in the brain.[8] The accepted hypothesis suggests that multiple primary neuronal impairments lead to a series of intracranial and extracranial changes, triggering a physiological cascade that leads to migraine symptomatology.[9]
Initial recommended treatment for acute attacks is with over-the-counter analgesics (pain medication) such as ibuprofen and paracetamol (acetaminophen) for headache, antiemetics (anti-nausea medication) for nausea, and the avoidance of migraine triggers.[10] Specific medications such as triptans, ergotamines, or calcitonin gene-related peptide receptor antagonist (CGRP) inhibitors may be used in those experiencing headaches that do not respond to the over-the-counter pain medications.[11] For people who experience four or more attacks per month, or could otherwise benefit from prevention, prophylactic medication is recommended.[12] Commonly prescribed prophylactic medications include beta blockers like propranolol, anticonvulsants like sodium valproate, antidepressants like amitriptyline, and other off-label classes of medications.[13] Preventive medications inhibit migraine pathophysiology through various mechanisms, such as blocking calcium and sodium channels, blocking gap junctions, and inhibiting matrix metalloproteinases, among other mechanisms.[14][15] Non-pharmacological preventive therapies include nutritional supplementation, dietary interventions, sleep improvement, and aerobic exercise.[16] In 2018, the first medication (Erenumab) of a new class of drugs specifically designed for migraine prevention called calcitonin gene-related peptide receptor antagonists (CGRPs) was approved by the FDA.[17] As of July 2023, the FDA has approved eight drugs that act on the CGRP system for use in the treatment of migraine.[18]
Globally, approximately 15% of people are affected by migraine.[19] In the Global Burden of Disease Study, conducted in 2010, migraine ranked as the third-most prevalent disorder in the world.[20] It most often starts at puberty and is worst during middle age.[21] As of 2016[update], it is one of the most common causes of disability.[22]
Migraine typically presents with self-limited, recurrent severe headaches associated with autonomic symptoms.[23][24] About 15–30% of people living with migraine experience episodes with aura,[10][25] and they also frequently experience episodes without aura.[26] The severity of the pain, duration of the headache, and frequency of attacks are variable.[23] A migraine attack lasting longer than 72 hours is termed status migrainosus.[27] There are four possible phases to a migraine attack, although not all the phases are necessarily experienced:[28]
Migraine is associated with major depression, bipolar disorder, anxiety disorders, and obsessive–compulsive disorder. These psychiatric disorders are approximately 2–5 times more common in people without aura, and 3–10 times more common in people with aura.[29]
Prodromal or premonitory symptoms occur in about 60% of those with migraine,[30][31] with an onset that can range from two hours to two days before the start of pain or the aura.[32] These symptoms may include a wide variety of phenomena,[33] including altered mood, irritability, depression or euphoria, fatigue, craving for certain food(s), stiff muscles (especially in the neck), constipation or diarrhea, and sensitivity to smells or noise.[31] This may occur in those with either migraine with aura or migraine without aura.[34] Neuroimaging indicates the limbic system and hypothalamus as the origin of prodromal symptoms in migraine.[35]
 |
 |
 |
 |
Aura is a transient focal neurological phenomenon that occurs before or during the headache.[30] Aura appears gradually over a number of minutes (usually occurring over 5–60 minutes) and generally lasts less than 60 minutes.[36][37] Symptoms can be visual, sensory or motoric in nature, and many people experience more than one.[38] Visual effects occur most frequently: they occur in up to 99% of cases, and in more than 50% of cases are not accompanied by sensory or motor effects.[38] If any symptom remains after 60 minutes, the state is known as persistent aura.[39]
Visual disturbances often consist of a scintillating scotoma (an area of partial alteration in the field of vision which flickers and may interfere with a person's ability to read or drive).[30] These typically start near the center of vision and then spread out to the sides with zigzagging lines, which have been described as looking like fortifications or walls of a castle.[38] Usually, the lines are in black and white, but some people also see colored lines.[38] Some people lose part of their field of vision known as hemianopsia while others experience blurring.[38]
Sensory auras are the second most common type; they occur in 30–40% of people with auras.[38] Often, a feeling of pins-and-needles begins on one side in the hand and arm and spreads to the nose–mouth area on the same side.[38] Numbness usually occurs after the tingling has passed with a loss of position sense.[38] Other symptoms of the aura phase can include speech or language disturbances, world spinning, and, less commonly, motor problems.[38] Motor symptoms indicate that this is a hemiplegic migraine, and weakness often lasts longer than one hour unlike other auras.[38] Auditory hallucinations or delusions have also been described.[40]
Classically the headache is unilateral, throbbing, and moderate to severe in intensity.[36] It usually comes on gradually[36] and is aggravated by physical activity during a migraine attack.[28] However, the effects of physical activity on migraine are complex, and some researchers have concluded that, while exercise can trigger migraine attacks, regular exercise may have a prophylactic effect and decrease frequency of attacks.[41] The feeling of pulsating pain is not in phase with the pulse.[42] In more than 40% of cases, however, the pain may be bilateral (both sides of the head), and neck pain is commonly associated with it.[43] Bilateral pain is particularly common in those who have migraine without aura.[30] Less commonly pain may occur primarily in the back or top of the head.[30] The pain usually lasts 4 to 72 hours in adults;[36] however, in young children frequently lasts less than 1 hour.[44] The frequency of attacks is variable, from a few in a lifetime to several a week, with the average being about one a month.[45][46]
The pain is frequently accompanied by nausea, vomiting, sensitivity to light, sensitivity to sound, sensitivity to smells, fatigue, and irritability.[30] Many thus seek a dark and quiet room.[47] In a basilar migraine, a migraine with neurological symptoms related to the brain stem or with neurological symptoms on both sides of the body,[48] common effects include a sense of the world spinning, light-headedness, and confusion.[30] Nausea occurs in almost 90% of people, and vomiting occurs in about one-third.[47] Other symptoms may include blurred vision, nasal stuffiness, diarrhea, frequent urination, pallor, or sweating.[49] Swelling or tenderness of the scalp may occur as can neck stiffness.[49] Associated symptoms are less common in the elderly.[50]
Sometimes, aura occurs without a subsequent headache.[38] This is known in modern classification as a typical aura without headache, or acephalgic migraine in previous classification, or commonly as a silent migraine.[51][52] However, silent migraine can still produce debilitating symptoms, with visual disturbance, vision loss in half of both eyes, alterations in color perception, and other sensory problems, like sensitivity to light, sound, and odors.[53] It can last from 15 to 30 minutes, usually no longer than 60 minutes, and it can recur or appear as an isolated event.[54] Many report a sore feeling in the area where the migraine was, and some report impaired thinking for a few days after the headache has passed. The person may feel tired or "hung over" and have head pain, cognitive difficulties, gastrointestinal symptoms, mood changes, and weakness.[55] According to one summary, "Some people feel unusually refreshed or euphoric after an attack, whereas others note depression and malaise."[56][unreliable medical source?]
The underlying cause of migraine is unknown.[57] However, it is believed to be related to a mix of environmental and genetic factors.[8] Migraine runs in families in about two-thirds of cases[23] and rarely occur due to a single gene defect.[58] While migraine attacks were once believed to be more common in those of high intelligence, this does not appear to be true.[45] A number of psychological conditions are associated, including depression, anxiety, and bipolar disorder.[59]

Success of the surgical migraine treatment by decompression of extracranial sensory nerves adjacent to vessels[60] suggests that people with migraine may have anatomical predisposition for neurovascular compression[61] that may be caused by both intracranial and extracranial vasodilation due to migraine triggers.[62] This, along with the existence of numerous cranial neural interconnections,[63] may explain the multiple cranial nerve involvement and consequent diversity of migraine symptoms.[64]
Studies of twins indicate a 34–51% genetic influence on the likelihood of developing migraine.[8] This genetic relationship is stronger for migraine with aura than for migraine without aura.[26] It is clear from family and populations studies that migraine is a complex disorder, where numerous genetic risk variants exist, and where each variant increases the risk of migraine marginally.[65][66] It is also known that having several of these risk variants increases the risk by a small to moderate amount.[58]
Single gene disorders that result in migraine are rare.[58] One of these is known as familial hemiplegic migraine, a type of migraine with aura, which is inherited in an autosomal dominant fashion.[67][68] Four genes have been shown to be involved in familial hemiplegic migraine.[69] Three of these genes are involved in ion transport.[69] The fourth is the axonal protein PRRT2, associated with the exocytosis complex.[69] Another genetic disorder associated with migraine is CADASIL syndrome or cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy.[30] One meta-analysis found a protective effect from angiotensin converting enzyme polymorphisms on migraine.[70] The TRPM8 gene, which codes for a cation channel, has been linked to migraine.[71]
The common forms of migraine are polygenetic, where common variants of numerous genes contribute to the predisposition for migraine. These genes can be placed in three categories, increasing the risk of migraine in general, specifically migraine with aura, or migraine without aura.[72][73] Three of these genes, CALCA, CALCB, and HTR1F are already target for migraine specific treatments. Five genes are specific risk to migraine with aura, PALMD, ABO, LRRK2, CACNA1A and PRRT2, and 13 genes are specific to migraine without aura. Using the accumulated genetic risk of the common variations, into a so-called polygenetic risk, it is possible to assess e.g. the treatment response to triptans.[74][75]
Migraine may be induced by triggers, with some reporting it as an influence in a minority of cases[23] and others, the majority.[76] Many things, such as fatigue, certain foods, alcohol, and weather, have been labeled as triggers; however, the strength and significance of these relationships are uncertain.[76][77] Most people with migraine report experiencing triggers.[78] Symptoms may start up to 24 hours after a trigger.[23]
Also, evidence shows a strong association between migraine and the quality of sleep, particularly poor subjective quality of sleep. The relationship seems to be bidirectional, as migraine frequency increases with low quality of sleep, yet the underlying mechanism of this correlation remains poorly understood.[79]
Common triggers quoted are stress, hunger, and fatigue (these equally contribute to tension headaches).[76] Psychological stress has been reported as a factor by 50–80% of people.[80] Migraine has also been associated with post-traumatic stress disorder and abuse.[81] Migraine episodes are more likely to occur around menstruation.[80] Other hormonal influences, such as menarche, oral contraceptive use, pregnancy, perimenopause, and menopause, also play a role.[82] These hormonal influences seem to play a greater role in migraine without aura.[45] Migraine episodes typically do not occur during the second and third trimesters of pregnancy, or following menopause.[30]
Between 12% and 60% of people report foods as triggers.[83][84]
There are many reports[85][86][87][88][89] that tyramine – which is naturally present in chocolate, alcoholic beverages, most cheeses, processed meats, and other foods – can trigger migraine symptoms in some individuals. Monosodium glutamate (MSG) has been reported as a trigger for migraine,[90] but a systematic review concluded that "a causal relationship between MSG and headache has not been proven... It would seem premature to conclude that the MSG present in food causes headache".[91]
Migraines may be triggered by weather changes, including changes in temperature and barometric pressure.[92][93]
A 2009 review on potential triggers in the indoor and outdoor environment previously concluded that while there were insufficient studies to confirm environmental factors as causing migraine, "migraineurs worldwide consistently report similar environmental triggers ... such as barometric pressure change, bright sunlight, flickering lights, air quality and odors".[94]

Migraine is believed to be primarily a neurological disorder,[95][96] while others believe it to be a neurovascular disorder with blood vessels playing the key role, although evidence does not support this completely.[97][98][99][100] Others believe both are likely important.[101][102][103][104] One theory is related to increased excitability of the cerebral cortex and abnormal control of pain neurons in the trigeminal nucleus of the brainstem.[105]
Sensitization of trigeminal pathways is a key pathophysiological phenomenon in migraine. It is debatable whether sensitization starts in the periphery or in the brain.[106][107]
Cortical spreading depression, or spreading depression according to Leão, is a burst of neuronal activity followed by a period of inactivity, which is seen in those with migraine with aura.[108] There are several explanations for its occurrence, including activation of NMDA receptors leading to calcium entering the cell.[108] After the burst of activity, the blood flow to the cerebral cortex in the affected area is decreased for two to six hours.[108] It is believed that when depolarization travels down the underside of the brain, nerves that sense pain in the head and neck are triggered.[108]
The exact mechanism of the head pain which occurs during a migraine episode is unknown.[109] Some evidence supports a primary role for central nervous system structures (such as the brainstem and diencephalon),[110] while other data support the role of peripheral activation (such as via the sensory nerves that surround blood vessels of the head and neck).[109] The potential candidate vessels include dural arteries, pial arteries and extracranial arteries such as those of the scalp.[109] The role of vasodilatation of the extracranial arteries, in particular, is believed to be significant.[111]
Adenosine, a neuromodulator, may be involved.[112] Released after the progressive cleavage of adenosine triphosphate (ATP), adenosine acts on adenosine receptors to put the body and brain in a low activity state by dilating blood vessels and slowing the heart rate, such as before and during the early stages of sleep. Adenosine levels are high during migraine attacks.[112][113] Caffeine's role as an inhibitor of adenosine may explain its effect in reducing migraine.[114] Low levels of the neurotransmitter serotonin, also known as 5-hydroxytryptamine (5-HT), are also believed to be involved.[115]
Calcitonin gene-related peptides (CGRPs) have been found to play a role in the pathogenesis of the pain associated with migraine, as levels of it become elevated during an attack.[10][42]
The diagnosis of a migraine is based on signs and symptoms.[23] Neuroimaging tests are not necessary to diagnose migraine, but may be used to find other causes of headaches in those whose examination and history do not confirm a migraine diagnosis.[116] It is believed that a substantial number of people with the condition remain undiagnosed.[23]
The diagnosis of migraine without aura, according to the International Headache Society, can be made according to the "5, 4, 3, 2, 1 criteria", which is as follows:[28]
If someone experiences two of the following: photophobia, nausea, or inability to work or study for a day, the diagnosis is more likely.[117] In those with four out of five of the following: pulsating headache, duration of 4–72 hours, pain on one side of the head, nausea, or symptoms that interfere with the person's life, the probability that this is a migraine attack is 92%.[10] In those with fewer than three of these symptoms, the probability is 17%.[10]
Migraine was first comprehensively classified in 1988.[26]
The International Headache Society updated their classification of headaches in 2004.[28] A third version was published in 2018.[118] According to this classification, migraine is a primary headache disorder along with tension-type headaches and cluster headaches, among others.[119]
Migraine is divided into six subclasses (some of which include further subdivisions):[120]
The diagnosis of abdominal migraine is controversial.[122] Some evidence indicates that recurrent episodes of abdominal pain in the absence of a headache may be a type of migraine[122][123] or are at least a precursor to migraine attacks.[26] These episodes of pain may or may not follow a migraine-like prodrome and typically last minutes to hours.[122] They often occur in those with either a personal or family history of typical migraine.[122] Other syndromes that are believed to be precursors include cyclical vomiting syndrome and benign paroxysmal vertigo of childhood.[26]
Other conditions that can cause similar symptoms to a migraine headache include temporal arteritis, cluster headaches, acute glaucoma, meningitis and subarachnoid hemorrhage.[10] Temporal arteritis typically occurs in people over 50 years old and presents with tenderness over the temple, cluster headache presents with one-sided nose stuffiness, tears and severe pain around the orbits, acute glaucoma is associated with vision problems, meningitis with fevers, and subarachnoid hemorrhage with a very fast onset.[10] Tension headaches typically occur on both sides, are not pounding, and are less disabling.[10]
Those with stable headaches that meet criteria for migraine should not receive neuroimaging to look for other intracranial disease.[124][125][126] This requires that other concerning findings such as papilledema (swelling of the optic disc) are not present. People with migraine are not at an increased risk of having another cause for severe headaches.[citation needed]
Management of migraine includes prevention of migraine attacks and rescue treatment. There are three main aspects of treatment: trigger avoidance, acute (abortive), and preventive (prophylactic) control.[127]
Modern approaches to migraine management emphasize personalized care that considers individual patient needs. Lifestyle modifications, such as managing triggers and addressing comorbidities, form the foundation of treatment. Behavioral techniques and supplements like magnesium and riboflavin can serve as supportive options for some individuals.[128] Behavioral techniques that have been utilized in the treatment of migraines include Cognitive Behavioral Therapy (CBT), relaxation training, biofeedback, Acceptance and Commitment Therapy (ACT), as well as mindfulness-based therapies.[129] A 2024 systematic literature review and meta analysis found evidence that treatments such as CBT, relaxation training, ACT, and mindfulness-based therapies can reduce migraine frequency both on their own and in combination with other treatment options.[129] In addition, it was found that relaxation therapy aided in the lessening of migraine frequency when compared to education by itself.[129] Similarly, for children and adolescents, CBT and biofeedback strategies are effective in decreasing of frequency and intensity of migraines. These techniques often include relaxation methods and promotion of long-term management without medication side effects, which is emphasized for younger individuals.[129] Acute treatments, including NSAIDs and triptans, are most effective when administered early in an attack, while preventive medications are recommended for those experiencing frequent or severe migraines. Proven preventive options include beta blockers, topiramate, and CGRP inhibitors like erenumab and galcanezumab, which have demonstrated significant efficacy in clinical studies.[130] The European Consensus Statement provides a framework for diagnosis and management, emphasizing the importance of accurate assessment, patient education, and consistent adherence to prescribed treatments. Innovative therapies of oral medications used to treat migraine symptoms, such as gepants and ditans, are emerging as alternatives for patients who cannot use traditional options.[131]
A 2024 systematic review and network meta analysis compared the effectiveness of medications for acute migraine attacks in adults. It found that triptans were the most effective class of drugs, followed by non-steroidal anti-inflammatories. Gepants were less effective than non-steroidal anti-inflammatory drugs.[132][133]
Calcitonin gene-related peptide (CGRP) is a neuropeptide implicated in the pathophysiology of migraines. It is predominantly found in the trigeminal ganglion and central nervous system pathways associated with migraine mechanisms.[134] During migraine attacks, elevated levels of CGRP are detected, leading to vasodilation of cerebral and dural blood vessels and the release of inflammatory mediators from mast cells. These actions contribute to the transmission of nociceptive signals, culminating in migraine pain. Targeting CGRP has emerged as a promising therapeutic strategy for migraine management.[medical citation needed]
"Migraine exists on a continuum of different attack frequencies and associated levels of disability."[135] For those with occasional, episodic migraine, a "proper combination of drugs for prevention and treatment of migraine attacks" can limit the disease's impact on patients' personal and professional lives.[136] But fewer than half of people with migraine seek medical care and more than half go undiagnosed and undertreated.[137] "Responsive prevention and treatment of migraine is incredibly important" because evidence shows "an increased sensitivity after each successive attack, eventually leading to chronic daily migraine in some individuals."[136] Repeated migraine results in "reorganization of brain circuitry", causing "profound functional as well as structural changes in the brain."[138] "One of the most important problems in clinical migraine is the progression from an intermittent, self-limited inconvenience to a life-changing disorder of chronic pain, sensory amplification, and autonomic and affective disruption. This progression, sometimes termed chronification in the migraine literature, is common, affecting 3% of migraineurs in a given year, such that 8% of migraineurs have chronic migraine in any given year." Brain imagery reveals that the electrophysiological changes seen during an attack become permanent in people with chronic migraine; "thus, from an electrophysiological point of view, chronic migraine indeed resembles a never-ending migraine attack."[138] Severe migraine ranks in the highest category of disability, according to the World Health Organization, which uses objective metrics to determine disability burden for the authoritative annual Global Burden of Disease report. The report classifies severe migraine alongside severe depression, active psychosis, quadriplegia, and terminal-stage cancer.[139]
Migraine with aura appears to be a risk factor for ischemic stroke[140] doubling the risk.[141] Being a young adult, being female, using hormonal birth control, and smoking further increases this risk.[140] There also appears to be an association with cervical artery dissection.[142] Migraine without aura does not appear to be a factor.[143] The relationship with heart problems is inconclusive with a single study supporting an association.[140] Migraine does not appear to increase the risk of death from stroke or heart disease.[144] Preventative therapy of migraine in those with migraine with aura may prevent associated strokes.[145] People with migraine, particularly women, may develop higher than average numbers of white matter brain lesions of unclear significance.[146]

Migraine is common, with around 33% of women and 18% of men affected at some point in their lifetime.[147] Onset can be at any age, but prevalence rises sharply around puberty, and remains high until declining after age 50.[147] Before puberty, boys and girls are equally impacted, with around 5% of children experiencing migraine attacks. From puberty onwards, women experience migraine attacks at greater rates than men. From age 30 to 50, up to 4 times as many women experience migraine attacks as men;[147] this is most pronounced in migraine without aura.[148]
Worldwide, migraine affects nearly 15% or approximately one billion people.[19] In the United States, about 6% of men and 18% of women experience a migraine attack in a given year, with a lifetime risk of about 18% and 43%, respectively.[23] In Europe, migraine affects 12–28% of people at some point in their lives, with about 6–15% of adult men and 14–35% of adult women getting at least one attack yearly.[149] Rates of migraine are slightly lower in Asia and Africa than in Western countries.[45][150] Chronic migraine occurs in approximately 1.4–2.2% of the population.[151]
During perimenopause symptoms often get worse before decreasing in severity.[152] While symptoms resolve in about two-thirds of the elderly, in 3–10% they persist.[50]

An early description consistent with migraine is contained in the Ebers Papyrus, written around 1500 BCE in ancient Egypt.[153]
The word migraine is from the Greek ἡμικρá¾±νίᾱ (hÄ“mikrÄÂÂníÄÂÂ), 'pain in half of the head',[154] from ἡμι- (hÄ“mi-), 'half' and κρá¾±νίον (krÄÂÂníon), 'skull'.[155]
In 200 BCE, writings from the Hippocratic school of medicine described the visual aura that can precede the headache and a partial relief occurring through vomiting.[156]
A second-century description by Aretaeus of Cappadocia divided headaches into three types: cephalalgia, cephalea, and heterocrania.[157] Galen of Pergamon used the term hemicrania (half-head), from which the word migraine was eventually derived.[157] Galen also proposed that the pain arose from the meninges and blood vessels of the head.[156] Migraine was first divided into the two now used types – migraine with aura (migraine ophthalmique) and migraine without aura (migraine vulgaire) in 1887 by Louis Hyacinthe Thomas, a French librarian.[156] The mystical visions of Hildegard von Bingen, which she described as "reflections of the living light", are consistent with the visual aura experienced during migraine attacks.[158]

Trepanation, the deliberate drilling of holes into a skull, was practiced as early as 7,000 BCE.[153] While sometimes people survived, many would have died from the procedure due to infection.[159] It was believed to work via "letting evil spirits escape".[160] William Harvey recommended trepanation as a treatment for migraine in the 17th century.[161] The association between trepanation and headaches in ancient history may simply be a myth or unfounded speculation that originated several centuries later. In 1913, the world-famous American physician William Osler misinterpreted the French anthropologist and physician Paul Broca's words about a set of children's skulls from the Neolithic age that he found during the 1870s. These skulls presented no evident signs of fractures that could justify this complex surgery for mere medical reasons. Trepanation was probably born of superstitions, to remove "confined demons" inside the head, or to create healing or fortune talismans with the bone fragments removed from the skulls of the patients. However, Osler wanted to make Broca's theory more palatable to his modern audiences, and explained that trepanation procedures were used for mild conditions such as "infantile convulsions headache and various cerebral diseases believed to be caused by confined demons."[162]
While many treatments for migraine have been attempted, it was not until 1868 that use of a substance which eventually turned out to be effective began.[156] This substance was the fungus ergot from which ergotamine was isolated in 1918[163] and first used to treat migraine in 1925.[164] Methysergide was developed in 1959 and the first triptan, sumatriptan, was developed in 1988.[163] During the 20th century, with better study design, effective preventive measures were found and confirmed.[156]
Migraine is a significant source of both medical costs and lost productivity. It has been estimated that migraine is the most costly neurological disorder in the European Community, costing more than €27 billion per year.[165] In the United States, direct costs have been estimated at $17 billion, while indirect costs – such as missed or decreased ability to work – is estimated at $15 billion.[166] Nearly a tenth of the direct cost is due to the cost of triptans.[166] In those who do attend work during a migraine attack, effectiveness is decreased by around a third.[165] Negative impacts also frequently occur for a person's family.[165]
Transcranial magnetic stimulation shows promise,[10][167] as does transcutaneous supraorbital nerve stimulation.[168] There is preliminary evidence that a ketogenic diet may help prevent episodic and long-term migraine.[169][170]
Statistical data indicates that women may be more prone to having migraine, showing migraine incidence three times higher among women than men.[171][172] The Society for Women's Health Research has also mentioned hormonal influences, mainly estrogen, as having a considerable role in provoking migraine pain. Studies and research related to the sex dependencies of migraine are ongoing, and conclusions have yet to be achieved.[173]
Disability classes for the Global Burden of Disease study (table 8)
| External audio | |
|---|---|